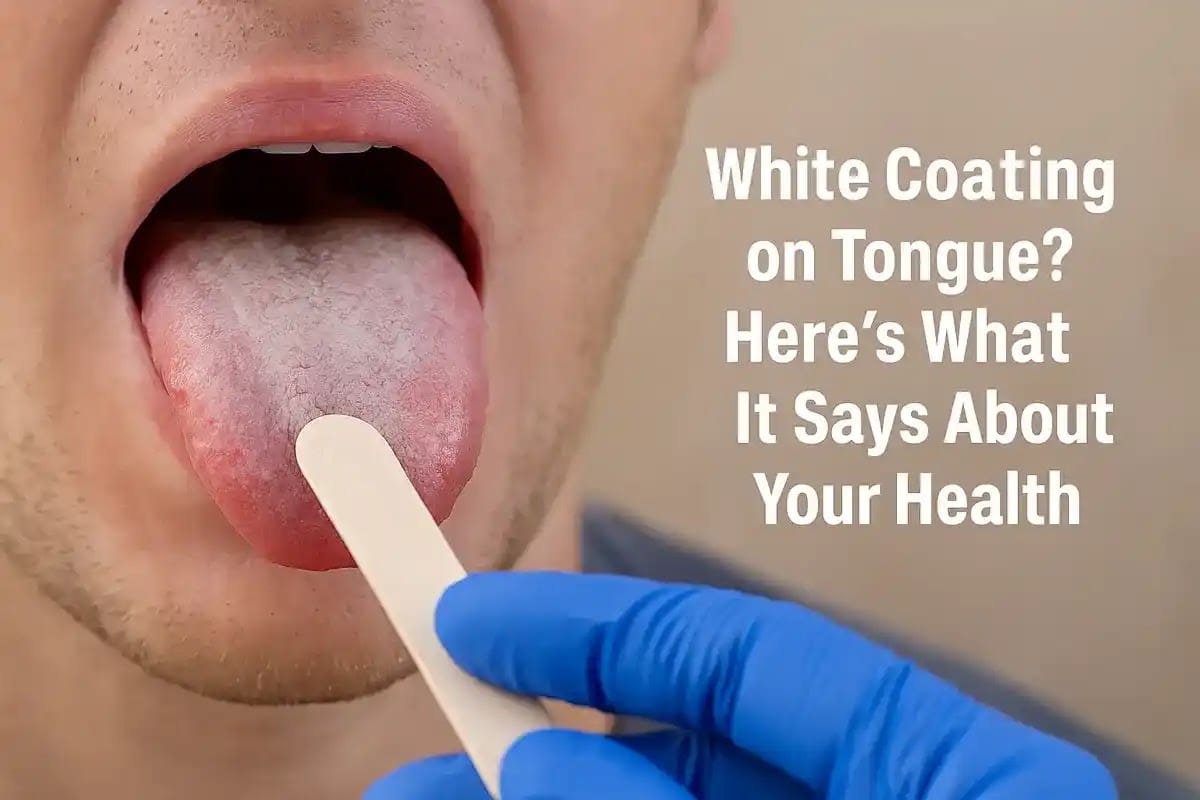
Introduction: When the Tongue Turns White
A healthy tongue is normally pink, moist, and evenly textured. When it turns white or patchy, it signals an imbalance in the mouth’s normal microbiology.
Oral thrush (oral candidiasis) is the most frequent cause of a white tongue. It results from overgrowth of Candida albicans, a fungal organism that lives harmlessly in small amounts within the mouth. When immunity or oral hygiene declines, this yeast multiplies and forms white patches.
A white tongue is not always thrush — but thrush almost always causes a white tongue.
Why Oral Thrush Happens
Small colonies of Candida normally exist in the mouth, kept under control by healthy bacteria and immune defenses. When that balance is disturbed, the yeast proliferates.
Common triggers include:
Antibiotic use: destroys protective bacterial flora.
Inhaled steroids: residues promote fungal growth if the mouth isn’t rinsed afterward.
Diabetes: high blood sugar feeds yeast.
Dry mouth: reduced saliva weakens antifungal protection.
Smoking or dirty dentures: encourage biofilm formation.
Weakened immunity: due to illness, chemotherapy, HIV, or chronic stress.
When these factors combine, Candida shifts from harmless resident to invasive pathogen, coating the tongue with a white, creamy layer.
Recognizing the Symptoms of Oral Thrush
Typical signs of white tongue and oral thrush include:
White or creamy patches on the tongue, inner cheeks, or lips that can be wiped off.
Redness or soreness beneath the patches.
Burning or discomfort during eating.
Loss of taste or a “cottony” mouth feeling.
Cracks at the corners of the mouth (angular cheilitis).
In severe cases, painful swallowing if the infection extends to the throat.
If symptoms persist for more than 10 days, consult a doctor or dentist for proper evaluation.
Diagnosis and Clinical Evaluation
Diagnosis of oral thrush is usually clinical. A healthcare provider examines the lesions and may perform:
Microscopic testing of an oral swab to detect fungal filaments.
Blood glucose testing to screen for diabetes.
Culture or biopsy if patches do not wipe off — to rule out leukoplakia or lichen planus.
Accurate identification ensures appropriate antifungal treatment and prevents recurrence.
Medical Treatment of Oral Thrush
A. Topical Antifungal Therapy (Mild Cases)
Nystatin oral suspension: rinse and swallow four times daily for 1–2 weeks.
Clotrimazole lozenges: dissolve one tablet five times daily for 14 days.
B. Systemic Antifungal Therapy (Severe or Recurrent Cases)
Fluconazole: 100–200 mg daily for 7–14 days under medical supervision.
Itraconazole oral solution: for resistant or recurrent infections.
C. Correcting Predisposing Factors
Control blood sugar in diabetes.
Rinse mouth after using inhaled steroids.
Clean and remove dentures nightly.
Avoid unnecessary antibiotics or corticosteroids.
With proper management, most cases improve within 3–5 days and resolve completely within two weeks.
Supportive Oral Care During Recovery
During treatment, supportive care helps relieve symptoms and prevent recurrence:
Rinse the mouth twice daily with warm salt water.
Maintain strict dental and tongue hygiene.
Avoid alcohol, tobacco, and spicy foods.
Drink plenty of water and eat balanced, nutrient-rich meals.
Good oral hygiene and hydration accelerate healing and restore microbial balance.
When to See a Doctor
Seek prompt medical attention if you experience:
White patches lasting longer than 10 days.
Pain, burning, or difficulty swallowing.
Recurrent thrush despite treatment.
Known diabetes, cancer therapy, or immune suppression.
White tongue with feeding difficulty in infants or elderly individuals.
Early intervention prevents complications and uncovers potential underlying disease.
Prevention and Daily Tongue Care
Your tongue plays a vital role in taste, digestion, and immune defense. Inadequate cleaning encourages bacterial and fungal buildup, leading to oral infections and bad breath.
Practical Tongue Care Tips
Gently clean your tongue daily with a scraper or soft-bristled toothbrush.
Stay hydrated throughout the day.
Avoid tobacco, excessive caffeine, and sugary foods.
Use an alcohol-free mouthwash if needed.
Replace your toothbrush every 2–3 months.
A clean, hydrated tongue is a reflection of overall systemic health.
Physician’s Summary
Oral thrush is completely curable when diagnosed early and treated appropriately. It is not just a cosmetic concern—it mirrors your immune health, metabolic balance, and oral hygiene.
Treat it promptly, complete the antifungal course, and maintain daily tongue care.
When your tongue turns white, it’s your body’s early warning signal — not one to ignore.
Frequently Asked Questions (FAQ)
Q1. Does a white tongue always mean oral thrush?
No. A white tongue may result from dehydration, smoking, or poor hygiene. Thrush patches typically wipe off, leaving a red surface beneath.
Q2. Can oral thrush be scraped away?
Only temporarily. The infection will recur unless antifungal treatment eliminates the underlying yeast. Avoid aggressive scraping.
Q3. How can I keep my tongue healthy?
Clean daily, stay hydrated, avoid tobacco and excess caffeine, and attend regular dental checkups.
Q4. Can oral thrush go away on its own?
Mild cases may subside briefly, but most require antifungal medication for complete recovery.
Q5. Is oral thrush dangerous?
In healthy adults, it is mild and manageable. In immunocompromised individuals, however, it can spread to the esophagus and requires urgent care.
Medical Disclaimer
This article is for educational purposes only and does not replace professional medical advice.
Always consult a licensed healthcare provider before starting or changing any medical treatment.